- Aging and diabetes
- The common symptoms of diabetes include –
- Probing Further: Fitness and Running with Diabetes
- Let’s first understand this disorder
- Running with Diabetes: Managing Blood Glucose Levels
- Assess your strength before you start running with diabetes
- Tips for running with diabetes
- Monitoring Blood Sugar and the Influence of Exercise on the Condition
- Effects on Insulin
- Safety tips for running with diabetes
- Cravings for sweets
- So, can you become a runner if you have diabetes?
- Scientific References & Further Reading
Before discussing running with diabetes, let us understand how aging and an unhealthy lifestyle can initiate the path of health deterioration. Sedentary choices – such as consuming junk and processed foods, irregular sleep patterns, alcohol abuse, and remaining seated for extended hours – will eventually take a heavy toll on the body. Most individuals fall into this behavioral category in their thirties and forties, often living with these habits as the years pass. Eventually, the consequences of these lifestyle choices manifest clearly: the body falls out of shape, and there is a noticeable loss of both strength and stamina.
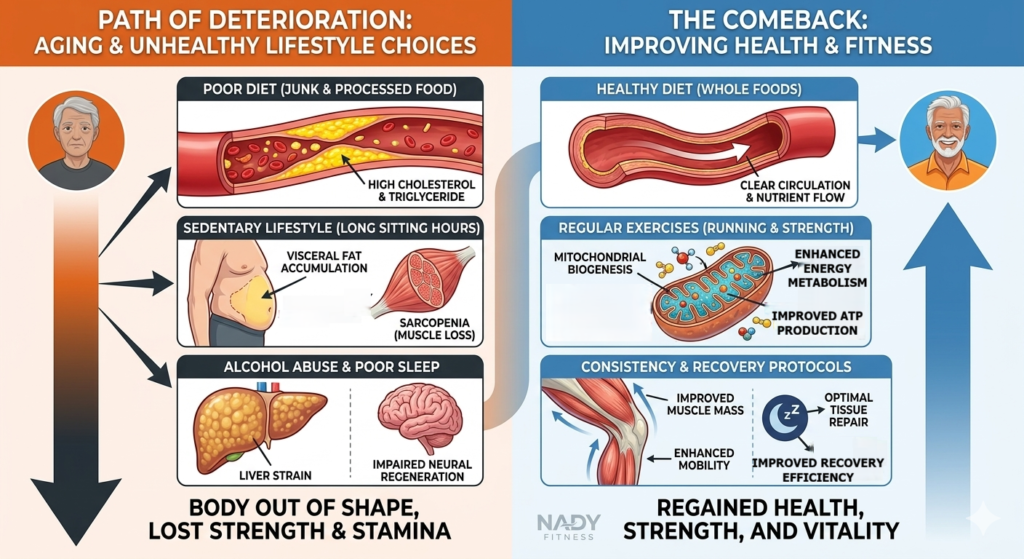
However, making a comeback and improving your health and fitness is still entirely possible. Your rate of progress will depend on the extent of the damage already sustained, as well as the consistency and frequency with which you counter it. To succeed, your focus must shift toward a disciplined diet and regular exercise. This requires implementing drastic changes to the lifestyle habits you may have grown accustomed to over the past decade or more.
Aging and diabetes
I have written extensively on how to improve health and fitness after 40; however, your fitness plan requires deeper customization if you are diagnosed with diabetes. Although this metabolic disorder can affect individuals at any age, it is significantly more prevalent among those between 45 and 65. Statistical data shows a clear upward trend in this age bracket, with positive diagnoses increasing from an average of 14.5% to 18.9%.
While specific data points may vary across different surveys, the consistent factor in all clinical studies suggests that the probability of a positive diagnosis increases with age. Furthermore, a staggering number of cases remain undiagnosed because people often fail to recognize or choose to ignore early warning signs, such as frequent urination and persistent thirst. Consequently, a substantial portion of the 40+ population is living with diabetes or prediabetes without even knowing it.
The common symptoms of diabetes include –
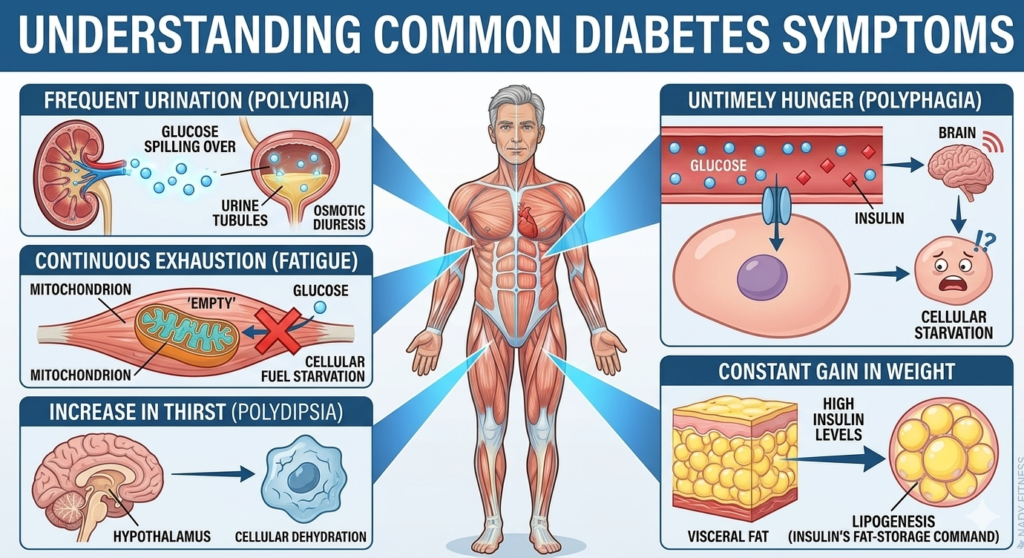
- Frequent urination
- Increase in thirst
- Continuous exhaustion
- Untimely Hunger
- Constant gain in weight
Probing Further: Fitness and Running with Diabetes
Returning to the intersection of fitness and diabetes for those aged 40 and beyond: frankly, I initially knew very little about this specific niche because I could not relate to it on a personal level. To bridge this gap in my understanding, I approached a close friend and neighbor who has undergone a profound transformation over the last 8-9 months by implementing radical lifestyle changes.
He has successfully shed more than 30kg and now appears visibly leaner and stronger. His remarkable progress even surprised his physician, who subsequently reduced his diabetes medication dosage by more than half. The physical change was so significant that he had to replace his entire wardrobe because none of his former clothes fit him anymore.
A big thank you my friend…
I could not think of a more qualified person to discuss this topic with, as he represents living proof that individuals with Type 2 diabetes can achieve elite levels of fitness if they commit to a structured plan. Though he wishes to remain anonymous and I cannot share his Instagram profile, he was gracious enough to sit with me and patiently answer all my technical questions.
We spoke at length about the current reality of the condition and the proactive steps that can be taken to halt its progression. The first critical insight he shared was the need for a shift in perspective: fitness for diabetics is a balancing act. One must work on physical improvement while ensuring blood sugar levels never fluctuate into dangerous territory – either too high or too low. While both extremes are hazardous, hypoglycemia (dangerously low sugar) can lead to immediate complications and can even be fatal.
The second pillar of his success was the absolute removal of sugar from his diet. However, he offered a silver lining: cutting out sugar does not necessarily mean sacrificing the enjoyment of sweets entirely. I will explain the nuance behind this at the end of this post.
Let’s first understand this disorder
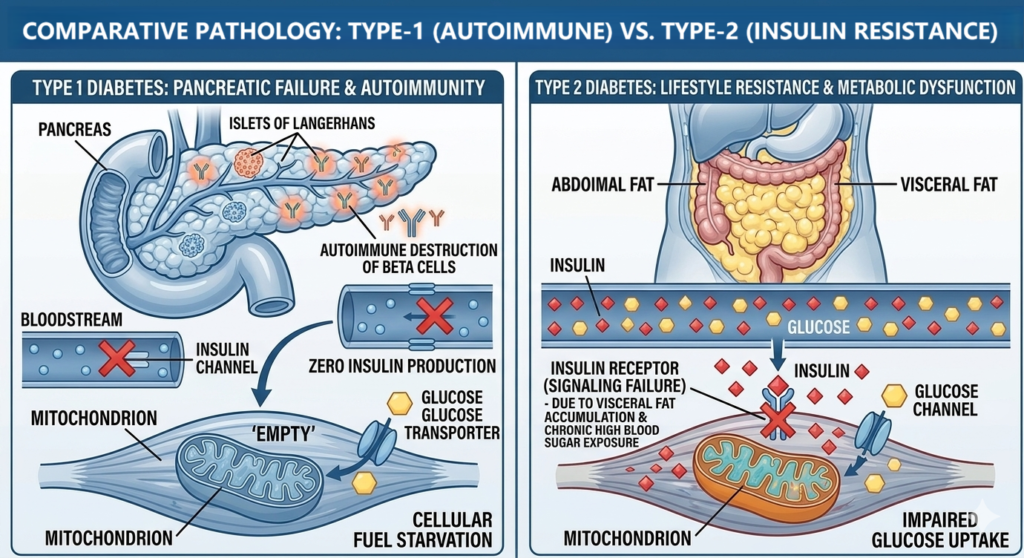
Diabetes is primarily classified into two types: Type-1 and Type-2. In Type-1 patients, the pancreas fails to secrete sufficient insulin; this condition is often autoimmune and can have a genetic component. Depending on the severity, a physician will typically prescribe insulin injections or the use of an insulin pump to manage glucose levels.
In contrast, Type-2 diabetes occurs when the body becomes resistant to insulin, often as a result of prolonged exposure to high blood sugar levels. For those diagnosed with prediabetes (typically characterized by an HbA1c level of up to 6.5%), it is possible to halt the progression of the disorder without daily medication. However, this requires a radical and disciplined shift in lifestyle.
The most effective way to lead a healthy life while running with diabetes is by adhering to a strict nutritional plan, staying consistently active, and maintaining blood sugar within a normal range at all times. It is important to note that individuals with fully developed diabetes will generally require lifelong medication to manage the condition effectively.
Running with Diabetes: Managing Blood Glucose Levels
Running is one of the most effective ways to maintain a healthy body and promote longevity. However, for those running with diabetes, it is critical to maintain a close watch on both blood glucose levels and heart rate. Modern technology, such as Continuous Glucose Monitors (CGM) and wearable heart-rate monitors, allows you to track these metrics in real-time, providing vital alerts when your levels fluctuate outside of a safe range.
Clinical studies indicate that glucose levels may deviate from your baseline average during or immediately after a run. These physiological changes typically occur approximately 30 minutes after the onset of your running routine. In many cases, this is a normal response to an increased metabolic rate, and levels often stabilize shortly after the session.
However, the risk profile changes based on your treatment plan. If you are already prescribed insulin or other hypoglycemic medications, the probability of significant blood glucose fluctuations – particularly hypoglycemia – is much higher. Conversely, if you are pre-diabetic and not currently on medication, the acute metabolic risks associated with running with diabetes are generally minimal, though monitoring remains a best practice.
Assess your strength before you start running with diabetes
My friend was very clear in his caution: generic running advice should not be given to individuals with diabetes, particularly those who have been sedentary for many years. According to his experience and observation, people living with diabetes often struggle with weight management; consequently, their knees and connective tissues may not initially be prepared to handle the high-impact rigors of a consistent running routine.
Even if you run, you could go for short sessions where you do not reach a state of complete exhaustion. A heart rate monitor will help you keep track of these exhaustion levels; it is a vital gadget for those running with diabetes. If you feel uncomfortable at any point, just stop running and follow the specific instructions of your doctor.
This advice is specifically for new runners, especially those struggling with weight gain. Once you develop the necessary strength in your muscles and joints, you can begin to increase the intensity of your runs. In fact, your body will eventually start to ask for more workouts. Just make sure that your heart rate and glucose levels are always in control. If you feel uncomfortable, just stop running and follow the instructions of your doctor. There is absolutely no reason why people with diabetes cannot follow their fitness goals. Running with diabetes can help in controlling the disorder and preventing it from progressing further.
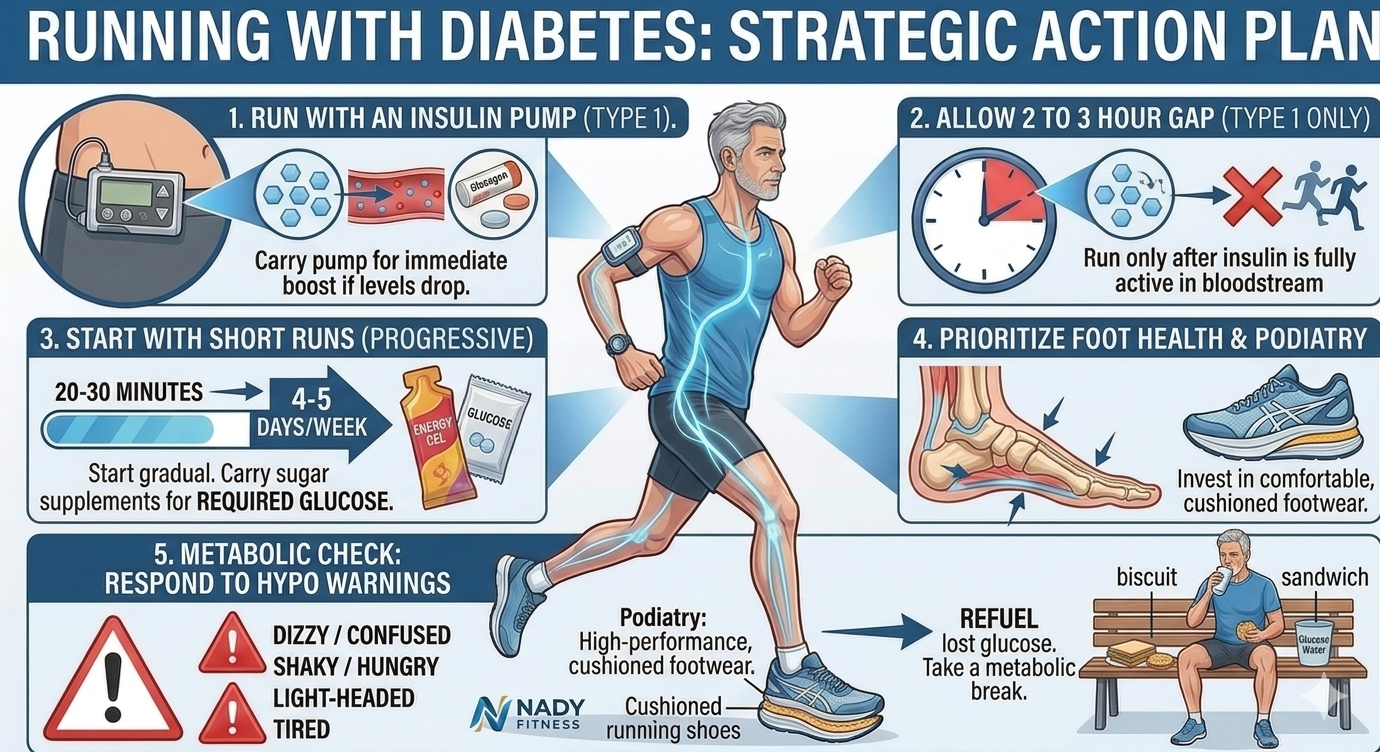
Tips for running with diabetes
- Monitor with a CGM: Use a Continuous Glucose Monitor (CGM) for real-time precision. Seeing the trend arrows (rising or falling) is the gold standard and is much more valuable than a single finger-prick number, allowing for proactive glucose refueling before a crash happens.
- Manage Your Insulin Pump (For Type 1): Ensure your pump is set to a “temp basal” or suspended if your CGM shows your levels are dropping. Always carry external glucose, as the pump itself cannot raise blood sugar.
- Give a Gap of 2 to 3 Hours (For Type 1): Avoid running while a recent insulin dose is at its peak absorption. This avoids “insulin stacking,” where the peak action of a bolus coincides with the peak intensity of the run – the #1 cause of sudden crashes.
- Take Short Runs: Start with 20–30 minutes for 4-5 days a week. This “test phase” helps you understand your metabolic floor and ceiling before committing to longer distances.
- Prioritize Foot Health: For the 40+ demographic, preventing blisters or pressure sores is essential, as diabetes can slow the healing process in the extremities. Use high-quality, well-fitted footwear and check your feet after every run for any signs of redness or irritation, as early detection is key for diabetic foot safety.
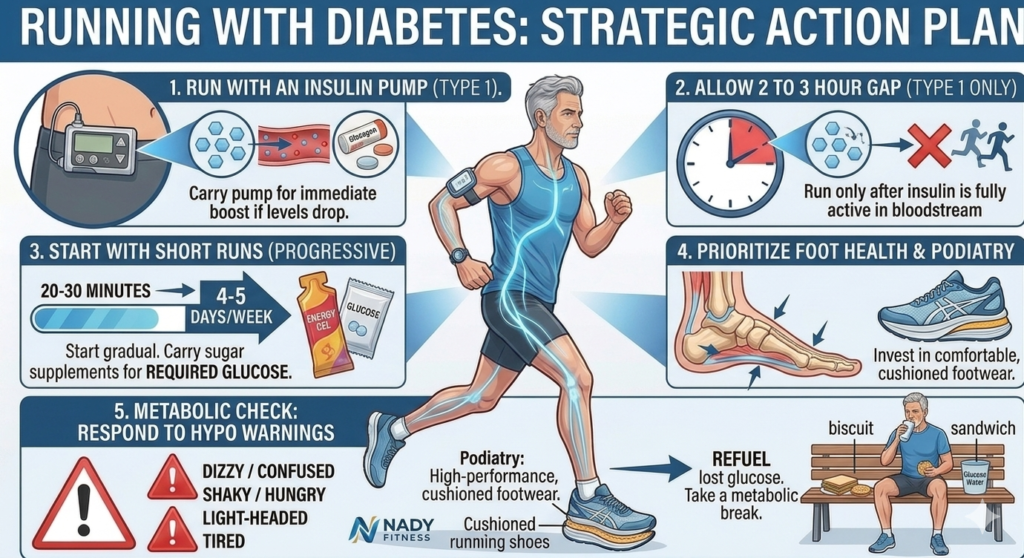
When you feel dizzy, hungry, tired, confused, shaky, or light-headed while running, you should take a break and relax for a while. You could have some glucose water and eat a sandwich or biscuit to refuel your body with the lost glucose levels.
Monitoring Blood Sugar and the Influence of Exercise on the Condition
People above 40 are prone to various disorders and health issues, such as back pain, joint pain, muscle tears, high blood pressure, and diabetes. Many of these conditions are curable with proper medical treatment or surgery; however, some disorders persist for a lifetime. One such condition is diabetes. Even though you cannot typically reverse the formal diagnosis, you can prevent it from progressing further by following a strict diet as suggested by your physician and maintaining a consistent exercise regime. Physical activities such as yoga, gym workouts, walking, swimming, jogging, brisk walking, cycling, mountain cycling, hiking, and trekking can all help you keep your diabetes at normal levels.
Benefits
- Improvement in health, fitness, and overall well-being.
- Healthy maintenance of blood-sugar levels.
- Lower chances of stroke and heart disease.
- Effective body weight management.
Exercising or maintaining physical fitness is not always easy for diabetes patients. Some individuals have suffered from sudden drops in their blood sugar levels either before or after exercise. Consequently, physicians suggest keeping a close eye on blood sugar levels while exercising with the help of proper monitoring devices.
Even though exercise is the best way to prevent the progression of diabetes, you should check which type of physical activity works best for your specific body. The best way to identify the right exercises for you is by monitoring your blood sugar levels both before and after your workout.
Effects on Insulin
Type-1 diabetic patients typically take insulin twice a day to maintain their blood insulin levels. This routine helps to avoid the dangers of glucose fluctuation in their blood. Such individuals require close attention to their blood glucose levels both before and after their exercising hours. However, regular glucose level checking is highly recommended for people who are diagnosed with Type-2 diabetes as well.
Physicians suggest a particular set of exercise regimes for people on daily insulin intake. Low blood sugar is known as hypoglycemia, and a higher glucose level is known as hyperglycemia. It is advisable to seek the help of your physician to understand the specific workout options that work for your condition. Besides exercising, you must follow a proper diet for the healthy maintenance of glucose levels; your physicians can also help with this.
Running and Diabetes
Running is excellent for maintaining a healthy glucose level and putting the required tension on the leg muscles. Studies have proved that people with Type-2 diabetes can reduce insulin resistance by running a few miles every day. Running is a flexible form of exercise because you can choose to sprint, go at a medium pace, or take it slow. Therefore, running with diabetes is highly feasible because it can be customized according to your individual strength and health condition. Each intensity level has different effects on blood sugar, so monitoring your response helps prevent the disorder from progressing.
Safety tips for running with diabetes
- Ensure you have plenty of glucose water: This is essential to keep your glucose levels in check and provide an immediate energy source.
- Monitor with a CGM: Instead of relying only on periodic checks, use a Continuous Glucose Monitor (CGM) for real-time precision. Watching the trend arrows allows for proactive glucose refueling as needed.
- Carry a Emergency Glucose/Glucagon Kit: If you run for over 60 minutes, carry a dedicated kit with fast-acting glucose or a Glucagon pen (if prescribed) to manage severe drops.
- Run with a partner: Going on a run with a partner helps to ensure your medical safety, especially when exploring new routes.
- Avoid Hypoglycemia: There are possibilities of experiencing hypoglycemia, which should be avoided at all costs. The drivers of this condition can be your current health status, pushing too hard, or skipping medication. This is why you should always monitor your heart rate while running and try to keep it within the permissible limits for your condition.
- Combat Dehydration: Running can sometimes lead to dehydration, and glucose water or electrolyte drinks can be your best combat measure in these instances.
A few things to remember for running with diabetes
- Monitor your blood sugar before starting exercise. If it is between 90 mg/dL and 250 mg/dL, you are generally good to go. If the number is 250 mg/dL or higher, you should not risk exercising, especially if your urine test confirms the presence of ketones. In such a case, you will need to work first on bringing down the blood glucose level to a safe range. On the lower side, you should not risk exercising if the glucose level is below 90 mg/dL.
- Keep something sugary or carbohydrate-rich with you. Have these items available on your workout sessions so you can consume them if your glucose level goes down during exercise.
- Start your exercise session after a snack or small meal. You should eat more if your exercise session goes beyond 60 minutes. This food should not interfere with your regular diet.
- Monitor blood sugar levels after the exercises. People may experience a blood sugar drop or rise from the normal level immediately after the sessions. It is normal, but it should stabilize when your body starts to rest. If not, follow your doctor’s instructions immediately.
The absorption mechanism of insulin in your body is different, which is why your exercise routines should be adjusted as per the condition. Diabetes is a disorder that can be diagnosed in people of various ages. However, a healthy diet and exercise routine can help you lead a stress-free and longer life.
Cravings for sweets
According to my friend, people with diabetes need not always sacrifice their cravings for sweets. Sugar is an absolute no, but there are many sugar-free products like ice creams and chocolates available these days. He suggests that having 1–2 fruits is okay, but not to juice them, and never on an empty stomach. Juicing will break down the fibers that are needed to slow down the absorption of sugar in the body.
You could have an occasional sweet if your heart desires, but don’t forget to monitor your glucose level. Also, avoid eating too many fast carbs like white rice and white bread. Absolutely avoid eating biscuits and other ready-to-eat snacks made from bleached flour (maida).
However, you should not take these things at their face value because product ads and labels can be deceiving. You must check all the ingredients that go into making these products. If you have any doubts regarding any ingredient, you must first discuss it with your doctor or dietitian.
So, can you become a runner if you have diabetes?

The answer is YES, and many people with diabetes run marathons. You can do running with diabetes, too, but you must closely monitor and manage your blood sugar and plan your diet accordingly. However, you must also take care of other diabetes management practices like proper hydration and strength training. You must keep an eye on your energy level, not only while running but also after the session.
Carry some snacks to refuel whenever you feel short of energy. You could start with a running partner to keep an eye on you and then go solo as you improve. Always inform someone if you are going on a long run and remember to take your medical identification. Running with diabetes is very much a possibility, but you should control the blood glucose levels at all times.
Scientific References & Further Reading
Clinical Resources: Exercise and Diabetes: Safety and Benefits – UPMC Children’s Hospital of Pittsburgh
Athletic Performance: The Complete Guide to Running with Diabetes – Runner’s World
Want professional content writing services to turn your ideas into engaging blog posts that your readers love?
Let’s build your authority in the fitness and health niche together.